Psychological and behavioural factors and risk for development of chronic pain syndrome in relation to neck injuries
Tatjana Sivik, Olle Bunketorp, Natasha Delimar, Rebecca Schoenfeld
Medical examination and treatment
Table 1. Correlations between length of sick-leave and psychosocial/work related variables.
Table 2. Discriminant function analysis of Work-APGAR, STAI, BDI and PTSD.
Figure 1. Regression analysis between length of sickleave and variable BDI.
Figure 2. Regression analysis between length of sickleave and variable STAI.
Figure 3. Regression analysis between length of sickleave and variable PTSD.
Chronic pain syndrome after necks injuries in traffic accident causes the society considerable costs in addition to the suffering of the victims. This study is an integrated part of a large study, evaluating the injury mechanisms, the diagnostic procedures, the treatment, and the prognosis of all types of neck-injuries in traffic accidents.
The purpose of the study was to investigate if there are any relationships between work related psychosocial factors and psychological (emotional) factors on the one hand and the risk for development of chronic pain syndrome following cervical spine distortions in traffic accidents on the other.
Method: In area of West Sweden all consecutive patients who reported traffic accident related to neck trauma were investigated within 2 weeks after the accident. One year following the investigation, a follow-up questionnaire was mailed to all participants. Those that returned a completed questionnaire were included in this study.
Results: Follow-up interview data were obtained from 282 patients (83% compliance) . Discriminant analysis revealed that those patients still on sick-leave at the one-year follow-up had significantly less favorable Work-APGAR scores and emotional state at the time of the initial investigation. Based on the data, a predictive discriminant model was identified.
Conclusions: The results of this study imply that work related psychosocial as well as general behavioral/emotional factors are related to the risk for development of chronic pain syndrome and that an integrative bio-psycho-social approach would be of advantage for the diagnosis and treatment of injured and traumatized patients at an early stage.
Key words: Neck injury, psychosocial work factors, persistent pain, emotional vulnerability, predictive, discriminant, STAI, BDI, PTSD.
ADDRESSES: The Traffic Injury Register, Department of Orthopaedics (Bunketorp O, MEng MD PhD Project leader), Östra Hospital, University of Göteborg, S-416 85 Gothenburg, Sweden and the Institute of Psychosomatic Medicine, Kvibergsvägen 5, S-415 05 Gothenburg, Sweden (Sivik T, MD PhD MA, Delimar N, PhD, Schoenfeld, R). Correspondence to Dr Olle Bunketorp or Dr Tatjana Sivik.
Introduction
The frequency of neck injuries reported as a result of road traffic accidents has increased during the last years. In the Scandinavian countries, the increase has taken an epidemic course and according to insurance companies (Länsförsäkringar AB, Sweden and Uni Storebrand, Norway) these injuries account for about 80% of the total costs for all traffic injuries. This might in part be due to increased traffic intensity, mainly in urban districts. In Gothenburg, the frequency of rear end collisions has increased almost threefold during the last ten years according to the local traffic authorities. Another explanation could be the more general use of seat belts, which is related to better survival but also to a greater risk for minor neck injuries1.
The major part of these injuries are classified as cervical spine distortions, so-called acceleration-deceleration injuries, most of which are caused by rear-end collisions, resulting in a whiplash trauma. According to a previous study in Gothenburg2, 50 percent of the injured recovered from symptoms during the first three months but 40 percent had symptoms after three years. About 15 percent had significant problems and were on sick leave over a year. Nygren3 has shown that ten percent of the injured in rear end collisions develop significant permanent impairment.
Several authors have demonstrated that some persons are more inclined than others to develop a chronic pain syndrome, irrespective of a connection with a known injury or an accident4-11. Psychiatric symptoms and post-traumatic disorders are common after road accident injuries12, and it seems therefore likely that vulnerable persons would be at a greater risk of developing disabling symptoms and disorders in connection to an accident4,5,7. Other factors may also be involved in the process. Recently, Awerbuch evaluated studies, published in English and derived from MEDLINE, that covered epidemiological, pathogenic and psychological aspects of whiplash trauma13. This review concludes that, at least in Australia, "Comparative studies suggest that "whiplash" is an illness reinforced by legal and social sanctions." Many authors also doubt that there are only organic reasons for persistent symptoms and suspect emotional factors or compensation neurosis as additional causes14.
It would be of great value to identify those individuals with risk factors for persisting problems at an early stage. There are several such factors as Evans15 and Amundson16 have noted in excellent overview articles. Older age of patients, previous neck-shoulder problems, degenerative spine disorders, cervical stenosis, the presence of inter scapular or upper back pain, occipital headache, objective neurological signs, neck stiffness and muscle spasm, insurance claim, and litigation are some. However, the risk factors are not unanimously agreed upon in the literature as was pointed out by Amundson16, and Evans15 stressed the need for further evaluation with prospective randomized studies.
Disabling psychiatric sequelae are important markers among those patients who develop a chronic pain syndrome in relation to the accident, while there is no evidence that the severity of the injury would be a sole reason of chronification. One important question is if there are any psychological and psychosocial factors associated with the prognosis. Radanov et al.17 investigated the personality structure of 78 neck-injured patients about a week after the accidents, and they found no significant psychological differences between patients with and those without remaining problems six months later. However, they found injury related cognitive impairment as predictive of persistent symptoms. A study presented by Salminen et al.18 showed that tenderness and pain in the neck and shoulder region was correlated with "Type A behavior". This might indicate that, indeed, there are psychological factors associated with persistent problems after neck injuries as many of these patients develop pain and tenderness in the neck-shoulder region.
The purpose of this study was to investigate if there are any relationships between work related psycho-social and general emotional psychological factors on the one hand and the risk for development of chronic pain symptoms following cervical spine distortions in traffic accidents on the other.
Patients and methods
This study is an integrated part of a large study, evaluating the injury mechanisms, the diagnostic procedures, the treatment, and the prognosis of all types of neck-injuries in traffic accidents. The study is conducted by The Traffic Injury Register, an organization affiliated to the Department of Orthopaedics, Östra Hospital, which has been established to investigate the causes and consequences of traffic accidents in general.
All patients who registered at the emergency departments of the two main hospitals in Gothenburg and who were complaining of neck pain following a traffic accident were offered a routine check-up by a special neck injury team organized by the Traffic Injury Register. The study was prospective with a one-year follow-up.
Inclusion criteria
The following inclusion criteria were used for those who entered the study:
• Age between 20 and 60 years.
• Not pregnant.
• Neck injury-AIS19 = 1.
• No significant injuries in other body regions.
• Ability to understand and speak the Swedish language.
• No previous neck and back problem causing more than two weeks on sick leave during the year before the accident.
• Living in the Gothenburg area.
Medical examination and treatment
A neck injury team examined all patients. Forty percent were investigated within 2 weeks, 80% within one month and the remainder within 3 months. The circumstances of the accident, previous medical history and work history were thoroughly investigated by a nurse with good experience of neck injured patients. At the same time, the nurse also checked all the answers of the psychological tests described below. A specialized physiotherapist made a thorough clinical examination and evaluated the mobility of the neck and shoulders. In cases with more pronounced symptoms, a medical examination was made by an orthopedic surgeon and a neurologist. Standardized radiological examinations of the cervical spine were made in all cases, including flexion-extension radiographs six weeks after the accidents or as fast as possible in those cases who were examined later. All interviews and examinations were made with standardized protocols. All patients were given a written neck/shoulder training-program at their first visit to the emergency department. Further training instructions were given by the physiotherapist. A soft collar was recommended during the first weeks and the patients were sent for regular treatment to one of 20 specially educated physiotherapists in the Gothenburg region in cases with more pronounced symptoms. The patients were recommended a medical check-up by their own doctor within a couple of weeks if the symptoms did not improve. Follow-up data was collected after one-year by means of a mailed 34-item questionnaire regarding quality of life. Informed consent was obtained in all cases.
Psychological analysis
The psychometric investigation at the first examination by the neck injury team included the following tests:
· State Trait Anxiety Inventory (STAI) 20
· Beck Depression Inventor (BDI) 21
· CIDI-PTSD interview22
· Work-APGAR, a one-factor solution of items included in the 6 factors in the Theorell Work Situation test23, measuring the individual's experience of control, demands, stress, influence, and social support at his/her work.
Statistics
In order to study the relationship between the length of sick-leave and the psychological/work-related variables a correlation analysis was performed. Discriminant function analysis of the variables tested was made between two groups: those who were and those who were not on sick-leave at the time of completing the follow-up questionnaire. Regression analyses was performed in order to determine the relationship between sick-leave and the psychological and work related psychosocial variables.
Results
The follow-up questionnaire was completed and returned by 282 (116 men and 166 women), which were 85% of the subjects. The mean age of these was 35,6 yr. (SD=11,1), with no significant age difference between the sexes.
In this context, we were particularly interested in analyzing the relationship between perceived work-situation and emotional states during the initial investigation and sick leave as reported in the one-year follow-up. There were significant differences noted between the two groups, those that were and those that were not on sick-leave one year following the accident.
There was a clear relationship between length of sick leave and the parameters measured. Length of sick leave was positively correlated to STAI, BDI, PTSD and perceived stress at work and demands, and negatively correlated to perceived control, stimulation, influence and social support (table 1).
The discriminant function analysis revealed that Work-APGAR, STAI, BDI and PTSD show good discriminant capacity between those who are and those who are not on sick-leave one year after the accident. Work-APGAR and BDI have the strongest impact (table 2).
Regression analysis of the relationship between sick-leave and the variables measured reveal that sick-leave is dependent upon all the measured variables. Thus the results show that low scores on BDI, STAI and PTSD are strongly related to low scores on sick-leave (fig 1, 2, 3). High scores on Work-APGAR are strongly related to low scores on sick-leave (fig 4).
Discussion
In this study, we observed a significant relationship between work related psychosocial variable, emotional state on the one hand and sick-leave on the other.
The only way to identify with full certainty what factors are involved in the development of the whiplash syndrome would be a strict prospective study of all persons involved in these types of accidents, which for obvious reason is almost impossible to conduct. This study does not fulfil these criteria as it includes only those patients who accepted a follow-up by the neck injury team. However, even though the investigated group in this study is selected, and the injured were examined at various times after the accident, the results are interesting. The study presented here is the closest we can come to the ideal study for the time being. It involves a thorough psychological, social, and somatic investigation of a consecutive group of injured patients in relation to detailed accident data and clinical and radiographic findings, which are to be reported separately. The standardized examinations were made within a month after the accident in 80 percent of the cases and a follow up was made after one year. A possible explanation to the high frequency of persons with remaining symptoms in this study may be that the symptom-free persons (of that reason) were less interested in answering the questionnaire. Eighteen percent did not send back the questionnaire despite repeated contacts.
Considering the total costs for the society due to neck injuries sustained in traffic accidents, and the sufferings of the victims, it seems to be of utmost importance to prevent the accidents in the first place - and to reduce the risk of injury by appropriate means in the vehicles. Improved head restraints are one important way. But this would certainly not be enough - accidents and injuries would still occur and cervical injuries are caused by a variety of trauma mechanisms and in accidents where an ideal neck restraint will have no effect. Further, many people would still remain anxious and tense and because of this and other reasons be at risk for the development of post-traumatic symptoms. They may also - and perhaps because of the anxiety - become involved in new accidents as has been noted in some cases in our study. Some of these victims are, according to this and other recent studies in psychosomatic research, prone to get stuck in a state of chronic pain because of a certain constellation of personality attributes and psychosocial conditions. It appears, of course, rational if these could be identified at an early stage and treated adequately with an integrative bio-psycho-social treatment besides from the somatic routine treatment. Such an approach should naturally be recommended for all kinds of patients, diseases and injuries - but particularly, perhaps, in the orthopedic field where the psychological components of the healing process in the patients earlier by tradition have been less obvious.
In conclusion, it is clear that early identification of individuals at risk for developing chronic pain syndromes following traffic related injury is of high value. Early identification and multidisciplinary integrative psychosomatic treatment of somatic, behavioral and work related psychosocial aspects can potentially significantly reduce length of sick-leave. This would lead to less suffering for the individual as well as significantly reduced health care costs for society at large.
We thank Marianne Berqvist, assistant at The Traffic Injury Register, for her devoted work during the study and for her ability to take good care of all the patients who worry for their many problems after the accidents. Other persons involved in the main study are Bengt Lind, Malin Lindh, Lars-Erik Linder and Carsten Byrn. We are very grateful for their contribution to the planning of the study. The study was fully supported by the insurance company Länsförsäkringar AB, Sweden.
REFERENCES
1. Deans G, McGalliard J, Rutherford W. Incidence and duration of neck pain among patients injured in car accidents. Br Med J, 1986; 292:94-5.
2. Olsson I, Bunketorp O, Blåder S, Lindh M, Markhede G, Romanus B. Nackbesvär efter bilolyckor. In: Asp K, ed. Proc. of VTIs och TFBs forskardagar, del 2. 113-26. 1988.Swedish Road and Traffic Research Institute, S-581 01 Linköping, Sweden, Report 561. (In Swedish)
3. Nygren Å. Injuries to car occupants - some aspects of the interior safety of cars. A study of a five year material from an insurance company. Acta Oto-Laryngologica 1984; (suppl 395). (Thesis)
4. Costa PJ, McCrae RR.Neuroticism, somatic complaints and disease: is the bark worse than the bite?. J Pers, 32:137-44, 1988.
5. Lipowski ZJ. Somatization: The concept and its clinical application. Am J Psychiatry, 145: 1358-68, 1988.
6. Goldberg DP, Bridges K. Somatic presentation of psychiatric illness in primary care setting. J Psychosom Res, 32:137-44, 1988.
7. Sivik T. Personality Profile and Psycho Social Status of Chronic Back Pain Patients, Advances in Idiopathic Low Back Pain, 8;14:317-22, 1993.
8. Sivik T, Gustafsson E, Klingberg-Olssson K. Differential Diagnosis of Low-Back Pain Patients; A simple Quantification of the Pain Drawing. Nord J Psychiatry, 46;1:55- 62, 1992.
9. Sivik T, Röjwall S, Gustafsson E, Klingberg-Olsson K, Wagner A, Delimar N. Relationship between Back Pain and Personality. Psychological Vulnerability as Risk Factors for Development of Chronic Back Pain. Nord J Psychiatry, 46;3:190-3, 1992.
10. Sivik T, Delimar D. Characteristics of Patients who attribute Chronic Pain to Minor Injury. Scand J Rehab Med, 26:27-31, 1994.
11. Klingberg-Olsson K, Sivik T. Tendency to Somatize, Personality Traits and Low Back Pain - Psychological vulnerability as Risk Factor for the Development of Chronic Back Pain. Advances in Idiopathic Low Back Pain, 6;3:191-5, 1993.
12. Mayou R, Bryant B, Duthie R. Psychiatric consequences of road traffic accidents. Br Med J, 307:647-51, 1993.
13. Awerbuch M. Whiplash in Australia: Illness or Injury? Med J Aust, 157:193-6, 1992.
14. Neck injury and the mind (edit.). The Lancet, 338:728-9, 1991.
15. Evans R. Some observations on whiplash injuries. Neurol Clin, 4:975-97, 1992.
16. Amundsson G. The evaluation and treatment of cervical whiplash. Current opinion in orthopedics, 5;II; 17-27, 1994.
17. Radanov BP, di Stefano G, Schnidrig A, Ballinari P. Role of psychosocial stress in recovery from common whiplash. The Lancet, 338:712-5, 1991.
18. Salminen J, Pentti J, Wickström G. Tenderness and pain in neck and shoulder in relation to Type A behaviour. Scand J Rheumatology; 20:344-50, 1991.
19. The Abbreviated Injury Scale. The American Association for Automotive Medicine. Morton Groove, Illinois, 1990.
20. Spielberger c: Manual for the State-Trait anxiety inventory STAI- form Y. Consulting Press: palo Alto, 1983.
21. Beck AT. Depression inventory. Philadelphia, PA: Center for cognitive therapy 1978.
22. American Psychiatric Association. Diagnostic and statistical manual of mental disorders, third edition (DSM-IIIr). APA, Washington, 1987.
23. Theorell T, Michélsen H, Nordemar R. Validitytesting of indices psychological demands, control possibility, social support, sleeping disturbancies and hidden and overt coping. Institutional report. IPM, Karolinska Institute, Stockholm, 1993. (in Swedish).
Tabells
Table 1. Correlations between length of sick-leave and psychosocial/work related variables.
|
|
SICK-LEAVE |
|
STAI |
,46 |
|
BDI |
,58 |
|
PTSD |
,32 |
|
STRESS |
,32 |
|
CONTROL |
-,28 |
|
STIMULATED |
-,26 |
|
INFLUENCE |
-,22 |
|
SOCIAL SUPPORT |
-,14 |
|
DEMANDS |
,17 |
Marked correlations are significant at p < ,05000
N=282 (Casewise deletion of missing data)
Table 2. Discriminant function analysis of Work-APGAR, STAI, BDI and PTSD.
|
|
F-VALUE |
p-level |
|
WAPG |
5,26 |
,023 |
|
STAI |
1,94 |
,16 |
|
BDI |
6,44 |
,01 |
|
PTSD |
,88 |
,35 |
Summary grouping: Sick-leave (2 groups: YES, NO) Wilks' Lambda: ,86 approx. F(4,120)=5,0923 p<,0008
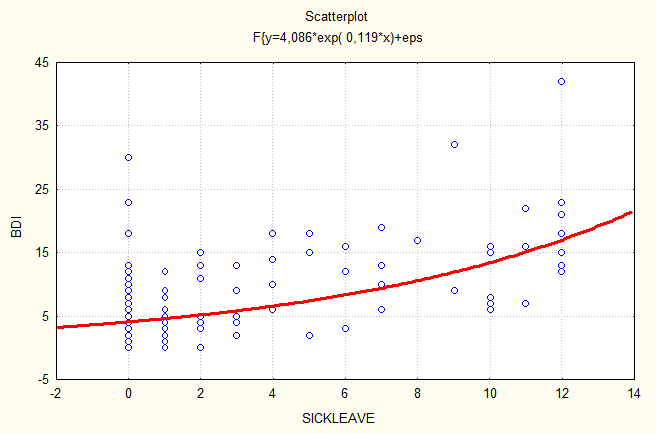
Figure 1. Regression analysis between length
of sickleave and variable BDI.
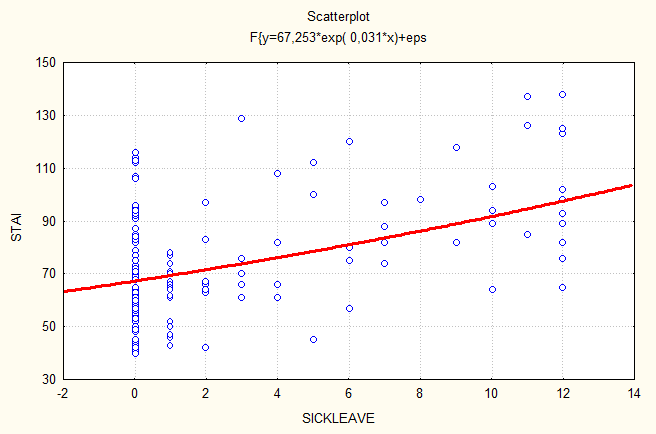
Figure 2. Regression analysis between length
of sickleave and variable STAI.
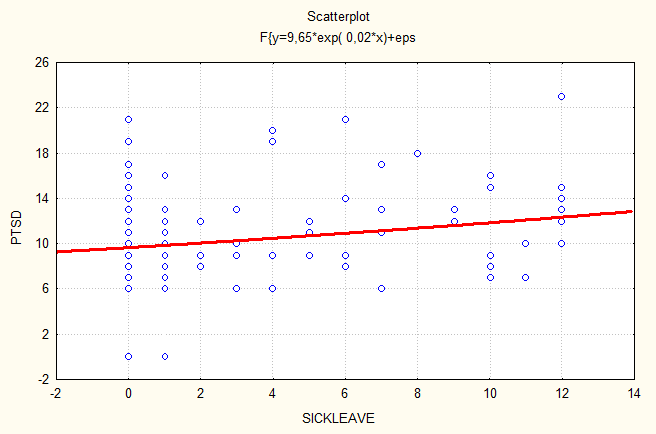
Figure 3. Regression analysis between length
of sickleave and variable PTSD.
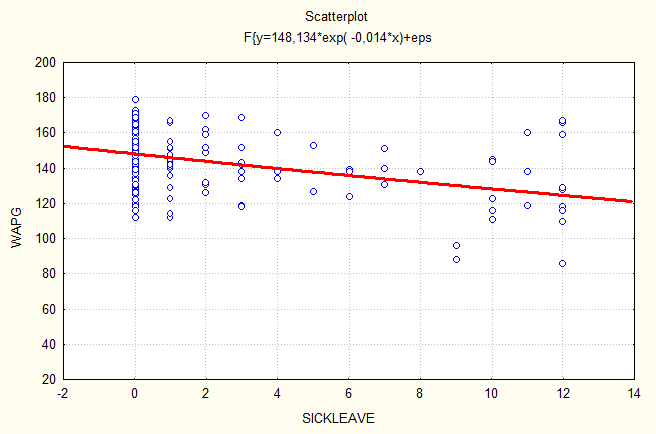
Figure 4. Regression analysis between length of sickleave and
variable Work-APGAR.